PAP TEST
A Pap test, publicly known as a Pap smear, is a test that detects cervical cancer in women. Cells from the cervix, the tip of the uterus, are collected and examined. If abnormal cells are found, they are tested to see if they are cancer or pre-cancer cells.
As to the American Society of Clinical Oncology, over 13,000 women are diagnosed with cervical cancer in the U.S. each year.
While that number is sobering, the rates for cervical cancer have dropped thanks to Pap testing, increased awareness of a group of viral infections called Human Papillomaviruses (HPV), and HPV vaccination.
HPV infection is the highest prevalent sexually transmitted infection (STI) in the U.S. and is the cause of most cervical cancers. Unfortunately, there is no cure or efficient treatment so far for HPV; however, there is a vaccine to help prevent infection.
The Centers for Disease Control and Preventions Advisory Committee on Immunization Practices (ACIP) has issued to following recommendations for HPV immunization:
- Regular vaccination at age 11 or 12 years but vaccination can be started as early as age 9
- Vaccination for females of age 13 to 26 years and males aged 13 through 21 years if they have not been not adequately vaccinated earlier
- Vaccination is recommended through age 26 years for gay, bisexual, and other men who have sex with men, transgender people, and people with compromised immune systems such as those with HIV who have not been adequately vaccinated earlier.
If you are sexually lively, your doctor will test for HPV when you have your Pap test or as part of a routine gynecological exam.
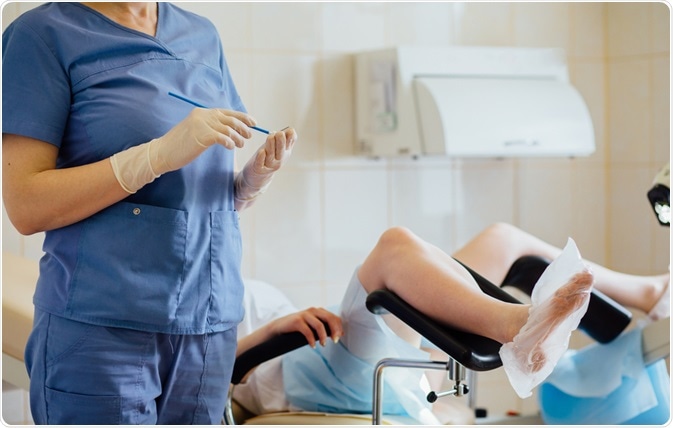
WHAT TO EXPECT DURING A PAP TEST
A Pap test is done in your doctor’s office. You will lie on an examination table with your feet in curved rests called stirrups during this examination. Then, your doctor will stick an instrument called a speculum into your vagina.
A speculum resembles a shoehorn or a duck’s bill and can be made of metal or plastic. It opens slightly so that your doctor can examine inside your vagina and can see your cervix. Speculums come in various sizes, and your doctor will choose a speculum that is an appropriate size for you.
The speculum may be coated in a lubricant to help move it smoothly and comfortably into your vagina.
Using a long swab, your doctor will gently scrape a small sample of cells from your cervix. You may feel an odd sensation, but this process is usually painless. Next, this sample is sent to a lab to be examined to look for any abnormal cells.
WHO SHOULD TAKE A PAP TEST, AND HOW OFTEN?
Back in 2018, the U.S. Preventive Services Task Force (USPSTF) recommended that women ages 21 to 29 have a PAP test once every three years and that women aged 30 to 65 have either a PAP test and HPV screen or both once every five years. However, PAP testing is not suggested for women under the age of 21 and over 65 who have had a history of negative PAP test results and negative HPV.
The American College of Obstetricians and Gynecologists and the American Society for Clinical Pathology note that these recommendations are for women who have never had signs or symptoms of cervical cancer, who have never had a previous diagnosis of a precancerous cervical lesion, women who have human immunodeficiency virus (HIV), women who were exposed to diethylstilbestrol (DES) in utero, and women who are at high risk for developing cervical cancer. If you fall in any of those groups, follow your doctor’s recommendations about how often you need a PAP test.
WHAT ARE THE POSSIBLE OUTCOMES OF A PAP TEST?
Results of a Pap smear can be expected, abnormal, or suspicious. If your Pap test is standard, it means there are no abnormal cells. Your doctor or the lab will send you the results, and you will not need another Pap test until your next regularly scheduled exam.
If your Pap test is abnormal, it may not mean that you have cervical cancer. If there are any atypical cells in your sample, the test is considered abnormal or positive. However, diagnosis depends on what type of abnormal cells are present.
A positive result doesn’t necessarily suggest you have a cervical tumor. What a positive impact means will rely upon the type of abnormal cells discovered in your test.
Possible abnormal results for a Pap test include:
- Atypical squamous cells of undetermined significance (ASCUS) — These cells are generally slightly abnormal in appearance. Their presence may indicate an HPV infection that can cause cervical cancer, and the sample will likely be tested again.
- Squamous intraepithelial lesion — These cells may be precancerous, and you may need additional examination and testing for a full diagnosis.
- Atypical glandular cells — These cells may or may not be pre-cancerous. Additional tests will likely be recommended for a more accurate diagnosis.
- Squamous cell cancer or adenocarcinoma cells — These cells generally mean there is cancer present in the cervix.
If your test results are not expected but not clearly abnormal, the sample may be tested again, or you may need to have a repeat Pap test within the following year.
WHAT HAPPENS IF THE RESULTS ARE ABNORMAL
If you have an irregular Pap test result, your doctor may recommend another diagnostic test called a colposcopy. This examination is performed in your doctor’s office and is much like a Pap test.
However, your doctor will use a magnifying scope (colposcope) to examine your vulva, vagina, and cervix more closely rather than taking a sample. A tissue sample may be taken and sent to the lab for testing and a more specific diagnosis if any anomaly is seen.
If you have a positive Pap test, you may have one or more of these diagnostic tests to rule out or confirm cervical cancer:
- Colposcopic biopsy — Your doctor will use a colposcope to view to remove a piece of tissue in the area where the tumor is suspected. Your doctor may use a local anesthetic to numb your cervix.
- Endocervical curettage (endocervical scraping) — Using a narrow instrument called a curette, inserted through your vagina and into the endocervical canal, the channel that leads from your outer cervix through your cervix and into your uterus, your doctor will take a sample of tissue from the endocervical canal for further lab testing and a more specific diagnosis.
- Cone biopsy (conization) — During this test, your doctor will remove a cone-shaped section of your cervix to test for cancer. This section is removed so that the doctor can examine and test deeper-level cervical cells for cancer. There are two ways the cone sample is usually taken, Loop electrosurgical procedure (LEEP, LLETZ) and cold knife cone biopsy. LEEP and LLETZ. It may be done in your doctor’s office, and your doctor uses a thin, heated wire instead of a blade to remove tissue for testing. A cold knife cone biopsy is done in the hospital or a surgery center, you will have medication to either put you to sleep (anesthesia) or to numb you from the waist down (epidural), and your doctor uses either a laser or small knife to remove the tissue sample. Both procedures can also be a form of treatment since your doctor may remove all the abnormal cells present in the cervix.
If you are diagnosed with cervical cancer, you will have treatment options based on how much cancer is present, how far into the cervix the cancer cells have grown, and if the tumor has spread to any other area in the uterus or the body.
The purpose of Pap testing is to identify cervical cancer as early as possible. The American Cancer Society reports that early-stage cervical cancer has a survival rate of 93%.
That’s why it?s essential for women between the ages of 21 and 65 to have routine testing at least once every three years.
If you find this article useful, please share it with your friends.