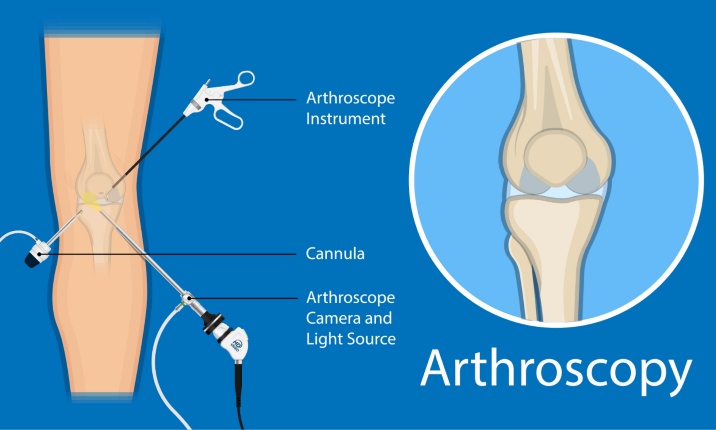
Arthroscopy
Arthroscopy is considered one of the great advances in joint surgery. It is a type of procedure that enables doctors to investigate, diagnose, and treat certain joint problems through a few small incisions.
Also familiar as minimally invasive or keyhole surgery, arthroscopy entails less post-operative pain and swelling, lower risks for developing an infection, and a quicker return to daily activities than traditional open surgery (which involves a large, long incision to give doctors wide access to a joint).
HOW IT WORKS
Arthroscopy uses incisions just large enough to accommodate long, pencil-thin surgical tools inserted into the body.
The arthroscope itself is a thin instrument that has a light and a tiny television camera on the end of it.
The camera sends live, illuminated images from inside the body to a television screen.
The surgeon can then see the bones, cartilage, muscle, ligaments, and tendons of a joint, enabling diagnosis and repair.
If necessary, other tools can be inserted through additional small incisions. The tools allow the surgeon to grasp, retrieve, cut, or shave tissue or bone or clean the field with suction.
WHEN IT IS USED
Arthroscopy is typically used for conditions that affect the knees, shoulders, elbows, ankles, hips, or wrists.
The procedure is valuable for diagnosis when other imaging tests, such as an MRI or CT scan, have not provided enough information.
Common procedures for which arthroscopy is effective include repairing torn cartilage or ligaments and removing loose bone fragments.
Conditions that can benefit from arthroscopy include joint damage, pain and swelling from arthritis, an injury like a torn meniscus in the knee, carpal tunnel syndrome in the wrist, frozen shoulder, a temporomandibular disorder in the jaw, a buildup of fluid that needs to be drained, or other joint pain or stiffness.
BEFORE SURGERY
Before your procedure, your doctor’s office will go over important information about the arthroscopy.
You should learn:
- where your procedure will be performed (arthroscopy is typically an out-patient procedure)
- what time you need to arrive at your surgery center
- when you should stop eating or drinking before the procedure
- which medications to stop taking before the procedure, and when you should stop taking them
- how long the procedure and post-surgical recovery will last
- what kind of pain you can expect immediately after surgery and during recovery
- which kinds of medications will be prescribed to treat pain, and when you should get them and take them
- whether physical rehabilitation will be necessary, and where you can go to get it
ON SURGERY DAY
After you arrive at the appointed time, you will be prepped for Arthroscopic surgery.
A health-care worker will insert an intravenous catheter (IV) into your arm or wrist so that you can be given a sedative to relax you before surgery.
You’ll then be wheeled (on a gurney) into an operating room and placed onto an operating table where the procedure will be performed.
Just before surgery begins, you may be given:
- general anesthesia (delivered through an IV) that renders you unconscious during the arthroscopy
- a local anesthetic (injected in the skin) to block the pain but keep you awake during the procedure
- a regional anesthetic (an epidural, delivered by injection in the spine) to numb half of your body but allow you to stay awake during the procedure
Once the procedure is underway, the surgeon will make small incisions around the joint.
The doctor will insert the arthroscope into the joint. Saline solution will be pumped into the joint so that it expands.
The expanded joint will provide improved visibility, giving the surgeon a better view of your body.
As the doctor performs your arthroscopy, the rest of the healthcare team (nurses and surgical assistants) will monitor your vital signs, such as your heart rate, blood pressure, breathing, and blood oxygen level.
At the end of the surgery, the doctor will close the incisions with either stitches or adhesive strips and then place a sterile bandage on the site.
WHAT TO EXPECT AFTER SURGERY
Most arthroscopic surgery is fast. Knee arthroscopy, as an example, usually lasts about an hour.
After your procedure, nurses will monitor you in a recovery room to ensure your vital signs are stable. After a few hours, you’ll likely be released to go home.
Once at home, you’ll be required to keep your incision and bandage dry. You will be able to take prescribed pain relievers. You may also be instructed to ice and elevate your joint.
If you have stitches, your doctor will remove them at a follow-up appointment. That is also when your doctor will determine when you’ll be able to take part in physical rehabilitation if it’s necessary.
It will most probably take a few days for your arthroscopy incisions to heal and several weeks or months for your joint to heal properly.
Longer incisions from traditional open surgery may require weeks to heal.
ARTHROSCOPY RISKS
Just because arthroscopy involves smaller incisions does not mean it’s risk-free.
Like with any other surgery, there is a risk of infection at the incision site or within the joint, tissue or nerve damage (which can cause temporary or permanent loss of sensation), or blood clumps that can develop in the legs or lungs.
It would help if you watched for potential warning signs immediately after surgery.
Those symptoms include numbness and tingling in the joint.
The arthroscopy was performed, fever, chills, increasing pain at the site of the incision or incisions, drainage at an incision, redness, excessive swelling, or bleeding.
However, arthroscopy is considered a low-risk procedure.
It has helped to reduce complications that normally occur in traditional open surgery.
Resources
Websites
“Arthroscopy.” Johns Hopkins Medicine Health Library. https://www.hopkinsmedicine.org/healthlibrary/test_procedures/orthopaedic/arthroscopy_92,P07676 (accessed October 15, 2018).
“Arthroscopy” Mayo Clinic. August 16, 2018. https://www.mayoclinic.org/tests-procedures/arthroscopy/about/pac-20392974 (accessed October 15, 2018).
“Arthroscopy.” OrthoInfo, American Academy of Orthopaedic Surgeons. May 2010. https://orthoinfo.aaos.org/en/treatment/arthroscopy/ (accessed October 15, 2018).