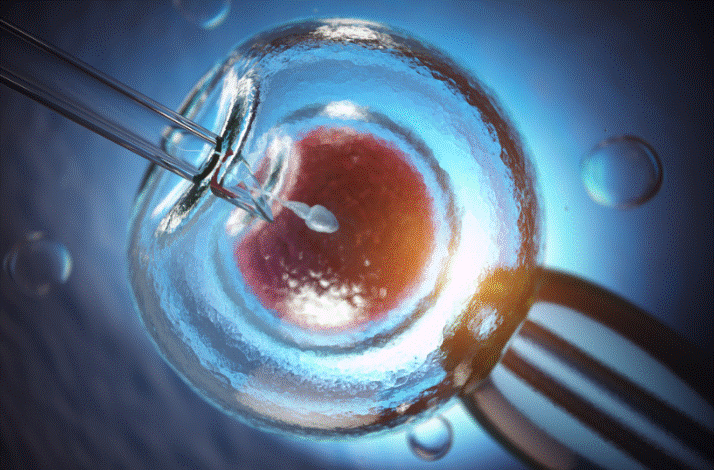
In Vitro Fertilization
In vitro fertilization (IVF) is a set of procedures to help couples who cannot conceive a child naturally or through other fertility treatments.
During IVF, eggs are extracted from the mother’s ovaries, a sperm sample is collected from the father, and the two are combined in a laboratory.
A fertilized egg (embryo) is then implanted in the mother’s uterus.
IVF is among the more reliable and effective forms of assistive reproductive technology.
Between 1987 and 2015, about one million babies were born in the U.S. through IVF or other assistive reproductive technologies.
GETTING STARTED
IVF starts with a consultation with a doctor who specializes in fertility. The doctor will review the personal and family health histories of the mother and father.
Diagnostic tests may be ordered, and physical examinations may be performed to help determine the cause of infertility and whether IVF is an appropriate approach.
An ultrasound of the mother’s ovaries may also be done.
Part of that initial consultation will include a discussion of your family goals, a review of several assistive reproductive options, along with a step-by-step explanation of the IVF process.
FERTILIZATION AND IMPLANTATION
After a couple has committed to IVF, the mother undergoes a series of hormone injections to stimulate egg production. This goes on for up to 20 days.
Every few days, an ultrasound of the ovaries is done to check the maturation of the mother’s eggs. The eggs grow in fluid-filled cysts called follicles.
Once the follicles grow to 18 millimeters in diameter, the mother receives injections of a different type of hormone to help complete the maturation of the eggs.
When the doctor determines the eggs are ready for extraction, he or she will use a hollow needle—injected through an area in the pelvic region—to retrieve the follicles and the eggs they contain.
The eggs are examined in a lab, and if the doctor determines there are enough healthy eggs to proceed, the eggs will be stored temporarily.
The father will then provide a semen sample. If the sperm from the sample is deemed healthy for fertilization, they will be united with eggs in a plastic dish containing a liquid solution designed to encourage cell growth.
It is called a “culture medium,” and scientists developed it to act in the same way as uterine fluid—the environment in which babies grow inside the womb.
The eggs are monitored to make sure fertilization has occurred, and cell division is ongoing.
After three to five days, one or more embryos will be implanted in the mother’s uterus. Doctors usually implant more than one embryo to help increase the chances of live birth.
WHO ARE GOOD CANDIDATES?
Couples who turn to IVF have usually tried other fertility procedures. A woman might receive hormones to boost egg production.
Or a couple might try intrauterine insemination, in which the father’s sperm is placed directly into the uterus around the time his partner is ovulating.
If these procedures aren’t successful, IVF may be a good option.
Fertility challenges have many causes, such as:
- Ovulation disorders. For many women, ovulation is infrequent, unpredictable, or is absent, making fewer eggs available for fertilization.
- Fallopian tube damage. The fallopian tubes carry eggs from the ovaries to the uterus. If a tube has been damaged or is blocked, it can make fertilization difficult.
- Endometriosis: This condition is characterized by the formation of uterine tissue outside of the uterus, potentially affecting the health and function of the ovaries, fallopian tubes, and uterus.
- Semen abnormalities: If sperm concentration is too low or sperm movement is weak, it can be difficult for sperm to fertilize an egg naturally.
In some cases, the reason for infertility can’t be explained. And for some couples who fear a serious genetic disorder may be passed on to their children, IVF allows doctors to screen the embryos for signs of the disorder.
Embryos containing no genetic markers of an inherited disorder may be implanted.
RISKS
It is not uncommon for an IVF pregnancy to result in multiple births if more than one embryo is implanted.
A pregnancy involving more than one baby, whether made possible by IVF or any means, raises the odds of premature birth and lower birth weight.
Other IVF risks include:
- Miscarriage: The chance of a miscarriage for a woman who uses IVF is about the same as that for a woman who conceives naturally. About 20 percent of all pregnancies end in miscarriage, which is defined as losing a pregnancy before the 20th week. The miscarriage rate tends to increase about maternal age.
- Ectopic Pregnancy: Less than five percent of women who use IVF experience an ectopic pregnancy, which occurs when the embryo implants in the fallopian tube and not the uterus. An embryo can’t survive outside the uterus, meaning there is no way to continue the pregnancy.
- Ovarian hyperstimulation syndrome: Many women using IVF are given fertility drugs, such as human chorionic gonadotropin (HCG), to help promote ovulation. In some cases, though, the drugs can cause ovarian hyperstimulation syndrome. It’s a condition in which the ovaries become swollen and painful. Symptoms tend to disappear within a week or so. However, if you become pregnant, symptoms may last for a few months.
- Stress: IVF can put financial and emotional strains on a couple. Reaching out to other IVF couples or support groups in your community may help ease the emotional challenges of this time in your life.
TAKEAWAY
It is important to remember that IVF doesn’t always work the first time.
According to “IVF by the Numbers” from Penn Medicine (see citation below), the “chance of having a full-term, normal birth weight and singleton live birth per ART [Assisted Reproductive Technology] cycle using fresh embryos from nondonor eggs is 21.3 percent for women younger than 35….”
Some couples go through multiple IVF procedures before having a successful pregnancy. At around $10,000 per IVF treatment (depending on your insurance coverage and the fertility center fees), it is not an inexpensive procedure.
But it has allowed thousands of couples to create families after there may have been doubts that such an outcome was possible.
Resources
Websites
“In Vitro Fertilization (IVF).” American Pregnancy Association. http://americanpregnancy.org/infertility/in-vitro-fertilization/ (accessed December 14, 2018).
“In Vitro Fertilization (IVF).” Johns Hopkins Medicine. https://www.hopkinsmedicine.org/gynecology_obstetrics/specialty_areas/fertility-center/infertility-services/ART-procedures/ivf.html (accessed December 14, 2018).
“In Vitro Fertilization (IVF).” Mayo Clinic. March 22, 2018. https://www.mayoclinic.org/tests-procedures/in-vitro-fertilization/about/pac-20384716 (accessed December 14, 2018).
“IVF by the Numbers.” Penn Medicine. March 14, 2018. https://www.pennmedicine.org/updates/blogs/fertility-blog/2018/march/ivf-by-the-numbers (accessed December 14, 2018).
“Miscarriage.” Mayo Clinic. July 20, 2016. https://www.mayoclinic.org/diseases-conditions/pregnancy-loss-miscarriage/symptoms-causes/syc-20354298 (accessed December 14, 2018).
Organizations
American Pregnancy Association, 3007 Skyway Circle N., Suite 800, Irving, TX, 75038, (800) 672-2296, info@americanpregnancy.org, http://americanpregnancy.org.
Society for Assisted Reproductive Technology, 1209 Montgomery Highway, Birmingham, AL, 35216-2809, (205) 978-5000, Fax: (205) 978-5018, sart@asrm.org, https://www.sart.org.