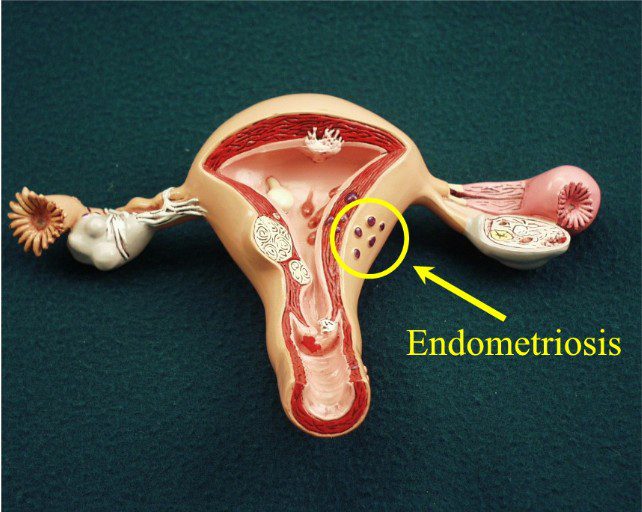
Endometriosis
Endometriosis is an illness in which tissue that commonly grows in the uterus to form the uterine inner lining (called the endometrium) grows outside the uterus.
It is a common condition—about 1 in 10 women of reproductive age (15–44 years old) are estimated to have endometriosis, according to the American College of Obstetricians and Gynecologists; according to the Office on Women’s Health, that means more than 6.5 million women in the United States have the condition.
Women with endometriosis often experience painful periods, heavy periods, pelvic pain between periods, and pain during sexual intercourse.
A woman with endometriosis can even have pain during bowel movements or urination if endometrial tissue has infiltrated her bowel or bladder.
The endometrial lining is what grows, sheds, and bleeds each time a woman has her period.
The tissue grows in response to estrogen during the cycle and sheds when estrogen levels drop, triggering a period.
This function is not location-dependent, meaning that even tissue outside the uterus will grow and bleed during a woman’s period.
Endometriosis can typically occur on the ovaries, fallopian tubes, the lining of the abdomen’s inner wall (called the peritoneum), or outer surfaces of the uterus (bladder, intestines, rectum).
Technically, but rarely, endometrial tissue can grow anywhere in the body, and it has been observed in the lungs, brain, and skin of some patients.
Bleeding from endometrial tissue in a non-uterine location can leave the blood with no way to escape the body (like it can through the vagina from the uterus); the trapped blood causes swelling and pain.
Healthy tissue surrounding the endometrial tissue outside the uterus can become irritated and inflamed.
Over time, scar tissue (called adhesions) can form on or around the endometrial tissue.
SYMPTOMS
Women with endometriosis can experience no symptoms, or they can experience severe pain; it depends on the severity of the disease.
Excruciating periods, chronic pelvic and lower back pain between periods, pain during or after sex, and painful bowel movements or urination, especially during a woman’s period, are common symptoms of endometriosis.
The pain can worsen over time, likely due to more endometrial tissue growing and more adhesions forming.
Bleeding or spotting between periods can occur with endometriosis, although other conditions and diseases can cause this symptom.
Stomach or digestive problems, such as constipation, diarrhea, nausea, or bloating, may also occur, especially during a woman’s period. Infertility may also indicate a woman has endometriosis, although there are multiple causes of infertility in women.
After menopause, endometriosis symptoms may improve due to the reduced amount of estrogen made in the body. Endometrial tissue then shrinks over time and causes fewer problems.
CAUSES
The cause of endometriosis is still largely unclear; ongoing research aims to uncover specific causes and markers to identify and diagnose it easily in the clinic successfully.
Although endometriosis can occur in any female who has a period, it seems to be more prevalent in women in their thirties and forties.
A variety of factors may impact a woman’s risk of having endometriosis, including having intervals lasting longer than seven days, having short menstrual cycles (fewer than 27 days), having a family member with endometriosis, having a disorder that blocks the normal flow of menstrual blood from the body, and not having had children.
PREVENTION
Although endometriosis cannot be prevented, a woman can lower her risk of developing it by making lifestyle choices that reduce her estrogen levels, ultimately reducing the endometrial tissue thickening.
Hormonal birth control can be used to control estrogen levels directly. Maintaining a low body fat percentage and exercising regularly (more than 4 hours per week) decreases the quantity of estrogen a woman’s body makes.
Avoiding large amounts of alcoholic and caffeine-containing beverages (more than one of each per day) can help avoid elevated estrogen levels in some women.
DIAGNOSIS
Women can only be officially diagnosed with endometriosis via laparoscopic surgery (called laparoscopy), during which the doctor looks in the pelvic area for endometrial tissue outside the uterus.
A biopsy may also be done; tissue samples may be taken during the laparoscopy and studied in the laboratory to determine if they are endometrial tissue.
However, endometriosis can be unofficially diagnosed by a doctor in other ways:
- A woman’s medical history, family history, and symptoms can suggest the diagnosis.
- A pelvic examination to feel for large cysts or scars behind the uterus can suggest endometriosis (although smaller patches of endometrial tissue are hard to feel via pelvic exam).
- An ultrasound can be used to identify ovarian cysts caused by endometriosis. An abdominal (also called uterine) or transvaginal ultrasound may be used to see the uterus and ovaries.
- Magnetic resonance imaging (MRI) may also be used to see the uterus and ovaries.
- Hormonal medicine, such as birth control and gonadotropin-releasing hormone (GnRH) agonists may be prescribed to see if they reduce pain. If a woman experiences less painful periods while taking hormonal medications, then she likely has endometriosis.
TREATMENT
As of 2019, there was no cure for endometriosis, only treatments to ease symptoms.
Endometriosis treatment depends on how severe the disease and symptoms are and whether the woman wants to have children.
There are two alternatives for treatment: medication and surgery. Medication is typically tried first, only resorting to surgery if needed.
POTENTIAL COMPLICATIONS
Other than the potentially severe pain, endometriosis may affect other aspects of a woman’s health.
Infertility
Although many women with endometriosis get pregnant, they may have a more difficult time doing so. Endometriosis is a main cause of infertility, with almost 40% of women with infertility also having endometriosis.
Endometrial tissue and adhesions may make it difficult for the sperm and egg to unite in the uterus or change the shape of the reproductive organs.
Sperm and eggs can be damaged by the inflammation caused by endometriosis.
The endometrial lining in the uterus may not develop normally, which makes implantation difficult or impossible.
Another factor is that the immune system may attack the embryo rather than implant it in the uterine lining and growing.
Links to other conditions
Links between endometriosis and other conditions have been seen in women and their families.
Such conditions include allergies; asthma; sensitivities to certain chemicals; autoimmune diseases, including lupus, multiple sclerosis, and some forms of hypothyroidism; chronic fatigue syndrome; fibromyalgia; and certain cancers, such as ovarian, breast, and the rare endometriosis-associated adenocarcinoma cancer.
Resources
Websites
“Endometriosis.” Mayo Clinic. March 23, 2019. https://www.mayoclinic.org/diseases-conditions/endometriosis/symptoms-causes/syc-20354656 (accessed August 5, 2019).
“Endometriosis.” MedlinePlus. March 22, 2019. https://medlineplus.gov/endometriosis.html (accessed August 8, 2019).
“Endometriosis.” Office on Women’s Health. April 1, 2019. https://www.womenshealth.gov/a-z-topics/endometriosis (accessed August 5, 2019).
“FAQ: Endometriosis.” American College of Obstetricians and Gynecologists (ACOG). January 2019. https://www.acog.org/Patients/FAQs/Endometriosis (accessed August 8, 2019).
Wadood Mohamed, Abdul, Valencia Higuera, and Matthew Solan. “Endometriosis.” Healthline. March 28, 2019. https://www.healthline.com/health/endometriosis (accessed August 6, 2019).
Organizations
American College of Obstetricians and Gynecologists (ACOG), 409 12th St. SW, Washington, DC, 20024-2188, (800) 673-8444, (202) 638-5577, https://www.acog.org .
Endometriosis Association, 8585 N. 76th Pl., Milwaukee, WI, 53223, (800) 992-3636, (414) 355-2200, Fax: (414) 355-6065, support@endometriosisassn.org, https://endometriosisassn.org .
Office on Women’s Health, U.S. Department of Health and Human Services, 200 Independence Ave. SW, Washington, DC, 20201, (800) 994-9662, (202) 690-7650, Fax: (202) 205-2631, https://www.womenshealth.gov .